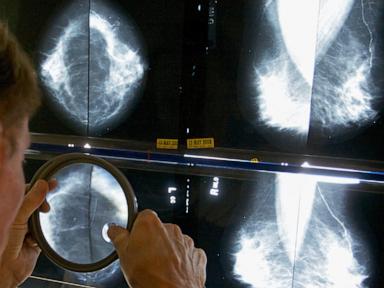
You turn 40, and suddenly your medical inbox floods with reminders. It is time for your first screening mammogram. Or is it?
If you ask three different medical organizations when to start getting breast cancer screenings, you will likely get three different answers. One group says 40. Another says 45. A third says it depends on your comfort level. It is a frustrating medical mixed message that leaves millions of women guessing about their own health. You might also find this connected coverage interesting: Stop Overthinking Anti Snoring Devices and Buy What Actually Works.
The confusion is real. It is driven by actual scientific debate over risks, benefits, and statistical math. Let's strip away the bureaucratic jargon and look at what the data actually says so you can make an informed choice with your doctor.
The Great Screening Debate
The primary source of the mixed messaging comes from a split between major health organizations. As highlighted in recent articles by Everyday Health, the results are worth noting.
The U.S. Preventive Services Task Force issued updated guidance that recommends women get screened every two years starting at age 40. Previously, they suggested waiting until 50 unless you had specific risk factors.
Meanwhile, the American College of Radiology and the Society of Breast Imaging advocate for annual screenings starting at age 40 for women at average risk. They push even harder for early risk assessments by age 25, especially for Black and Ashkenazi Jewish women, who face higher risks of aggressive, early-onset cancers.
Then there is the American Cancer Society. Their stance sits right in the middle. They recommend annual screenings starting at 45, with the option to start at 40 if you want to. They suggest switching to every two years once you hit 55.
No wonder you are confused.
Why Experts Do Not Agree on Mammogram Guidelines
Why can't the smartest minds in medicine just pick a number? Because screening is not a zero-sum game. Every medical test carries a balance of benefits and harms.
The benefit of a mammogram is obvious. It catches cancer early when it is easiest to treat. Early detection saves lives.
The harms are less talked about but heavily weighed by public health statisticians. The biggest issue is false positives. This happens when a mammogram finds something suspicious that turns out to be completely benign.
A false positive sounds like a minor inconvenience on paper. In reality, it means terrifying phone calls, stressful follow-up appointments, extra radiation from diagnostic mammograms, and invasive needle biopsies.
About half of all women who get annual mammograms for a decade will experience a false positive. For younger women in their 40s, dense breast tissue makes false positives even more common. Their tissue looks white on a mammogram, and so do tumors. Spotting a lump is like trying to find a snowman in a blizzard.
There is also the issue of overdiagnosis. Mammograms catch everything, including slow-growing, microscopic cancers that might never grow, spread, or harm you during your lifetime. Once found, doctors must treat them. This leads to surgeries, radiation, and chemotherapy for tumors that never actually posed a threat.
Public health groups look at the data across the whole population. They ask if the number of lives saved outweighs the thousands of unnecessary biopsies and panic attacks. Different groups look at that exact same data and draw different lines in the sand.
Calculate Your Own Personal Risk
Generic guidelines are built for the average person. But you aren't a statistic. Your personal risk profile matters far more than a blanket recommendation from a government task force.
Average risk means you have no personal history of breast cancer, no strong family history of the disease, and no genetic mutations like BRCA1 or BRCA2. It also means you haven't received high-dose radiation therapy to your chest during childhood or young adulthood.
If you fit that description, starting at 40 or 45 is a personal choice based on your tolerance for anxiety versus your desire for early detection.
If you are at high risk, the standard guidelines do not apply to you at all. You need a customized screening plan. This often means starting much earlier than 40. It frequently involves adding breast MRIs or ultrasounds alongside your yearly mammogram.
You are high risk if you have a first-degree relative—a mother, sister, or daughter—diagnosed with breast cancer, especially if they were diagnosed before age 50. Genetic mutations change the math entirely too.
The Density Factor
Your breast density changes how effective a mammogram is. Dense breast tissue is incredibly common. It isn't something you can feel during a self-exam. Only a mammogram can determine your density level.
If your radiologist notes that you have dense breasts, a standard 2D mammogram might miss smaller lumps. You should ask for a 3D mammogram, also known as digital breast tomosynthesis.
3D mammography takes images from multiple angles to create a layered view of the tissue. It makes it much easier to see through dense layers. Many insurance plans cover 3D mammograms now, but check your coverage first to avoid surprise bills.
How to Navigate the System Right Now
Do not wait for a doctor to bring this up. Take control of the timeline yourself.
Schedule a dedicated risk assessment discussion with your primary care provider or gynecologist by the time you turn 30. If you are Black or have a family history of cancer, do this in your mid-20s. Walk through your family medical history in detail. Ask your doctor to calculate your lifetime risk score using tools like the Tyrer-Cuzick model.
If your lifetime risk is under 15%, you are average risk. Look at the options. Decide if you want the aggressive approach of annual testing at 40, or if you prefer to wait until 45 or 50 to minimize the chance of false alarms.
If your lifetime risk is 20% or higher, work with a specialist to map out an advanced screening schedule immediately.
When you do book an appointment, go to an imaging center that specializes in breast health. Their radiologists read thousands of these scans a day. They are far better at spotting real issues and ignoring the fake ones.
Always request your actual imaging reports. Read the findings yourself. Look for your breast density score. Keep a digital folder of your records so you can bring them with you if you ever change healthcare systems. Consistency matters because radiologists love to compare your current scan against your old ones to see if anything has actually changed over time.